In Their Own Words: How HIV and AIDS Changed the Lives of 3 Kansas Citians Experiences vary, but stigmas remain
 Anjie Keyes’ life changed when she was diagnosed with HIV. (Emily Woodring | Flatland)
Anjie Keyes’ life changed when she was diagnosed with HIV. (Emily Woodring | Flatland)
Published November 17th, 2022 at 6:00 AM
Anjie Keyes’ life changed at 11:30 a.m. on June 30, 1995.
At the time Keyes, a young 20-something, had just landed a new job with the city of Kansas City, Missouri. A few days into her new gig, she felt sick.
Once her new health insurance kicked in, Keyes scheduled a doctor’s appointment to be tested. Then Keyes was called back to the clinic. When she arrived, the young doctor was crying.
“(The doctor) said, ‘I’m trying to pull myself together. … This is my first time having to tell someone, especially a Black female, about having HIV’,” Keyes recalled.
She was angry, in disbelief, and insisted they test her again. But the physician gently told her that what was on the paper was correct.
“I walked out of there feeling like I was so different,” said Keyes, her voice cracking.
Each time Keyes recounts the moment, she’s transported back to the clinic, then home where she sat in silence by herself.
By the 1990s, nearly 95% of the U.S. population had heard of AIDS, according to a Gallup Poll. Such widespread public awareness also fostered fear and stigma.
So much so that Keyes’ doctor warned her not to tell anyone, out of concern for her own safety.
Keyes, who turns 64 this December, has been living HIV-positive for over 27 years.
Keyes now encourages women living with HIV “to emerge, not just live. Emerge.” Over the years, there has not been as much support for people like her. Keyes wants to change that.
In the U.S., Black women now account for 54% of HIV diagnoses, according to the latest Centers for Disease Control and Prevention (CDC) “HIV Surveillance” data.
Black women account for 64% of 300 females living with HIV in Kansas City, according to a Missouri Health Department study from 2018.
Misconceptions and confusion about the risks for straight women clouded her ability to see the truth, she said.
One piece of Keyes’ story is how much she recognized correct information could have changed her outcome. Information is power.
Stigma’s Evolution
In 1981, the CDC announced the HIV and AIDS epidemic. Ten years later, education and public health campaigns swept the globe.
The need to stop misinformation was great.
People were being attacked, or ousted from families and communities. At one point, the general public thought a person with HIV could spread the virus with a hug or touch of a hand.
Virologists and infectious disease experts united. Celebrities stepped up. Community organizations mobilized. Advertising councils poured resources into campaigns.

Even though the risks of HIV and AIDS became better known in popular culture in the 1990s, stigmas and discriminatory behaviors persisted.
Communities of color, rural residents and the poorest folks were hardest hit. People without health insurance or easy access to a doctor would delay testing.
All too often in the early days of the epidemic, people would learn of their diagnosis too late. This sparked a movement to spread the message and focus on humanity.
Then, the popularity of shows such as “Pose” and Broadway hits like “Rent” put a spotlight on the epidemic, reframing the narrative from mere statistics into real lives.
One result has been evolving public perception.
Even though the urgency of messaging around HIV/AIDS has since waned, advocates say the need to support communities affected by HIV and AIDS is still present.
For context, in 1987 AIDS was considered the most urgent health problem by 62% of respondents, according to a Gallup Poll. This year, for the first time, one other illness broke the record, when 69% cited COVID-19.
“It’s easier to talk about COVID than it is to talk about HIV,” said Ithar Hassaballa, a public health and health equity scholar at the University of Kansas Medical Center.
Behaviors are shaped by taboos and available information.
She’s seen how wellness outcomes are affected by public perception. Broadly speaking, she said public health disparities are often rooted in other issues such as economic status, housing and other health factors such as one’s ZIP code.
“Access to care, access to social support really matters,” Hassaballa said. “There’s just a lot of work that needs to be done in terms of us seeing this as a health issue.”
Another key is funding research, which she said helps build understanding with people at the heart. She said people living with the virus should be central to the discussions and community research.
It paints a picture that can inform policies at a federal level.
Researchers see disparities that were present in those early days are showing up in new ways now. At the height of the COVID pandemic, the American Journal for Bioethics noted overlapping health issues and a lack of attention in HIV/AIDS research.
“The U.S. continues to be a leading country in the world for criminalizing people living with HIV, as well as, migration, sex work, drug use, and poverty,” the entry reads.
“The first letter in HIV stands for Human; HIV molecules are connected to people, people who live in the social world, with rights and dignity.”
Just last year, the CDC’s Vital Signs Report highlighted inequities that have persisted among gay men for over a decade.
The CDC’s report revealed another troubling trend — infections among Black and Latino gay men continued at around the same rate, while infections among white gay men declined.
Disparities also exist in treatment. The racial demographic of people who are prescribed medication to reduce chances of contracting HIV skews white.
Dr. Ume Abbas, an infectious disease physician at University Health, said it’s complicated.
“That was a sticky wicket for a long time because insurers were not ready to pay,” Dr. Abbas said.
“The other barrier was not only just cost. It was finding a provider to prescribe it.”
Studies consistently show Black people and Latinos are disproportionately affected, either with delayed diagnosis or treatment. Two of the main factors are cultural competency and medical mistrust.
The federal department of health has even acknowledged that people who need treatment most are not getting it. Abbas said treatment is key.
“Treatment is prevention as it blocks transmission of virus from infected to susceptible person,” she said.
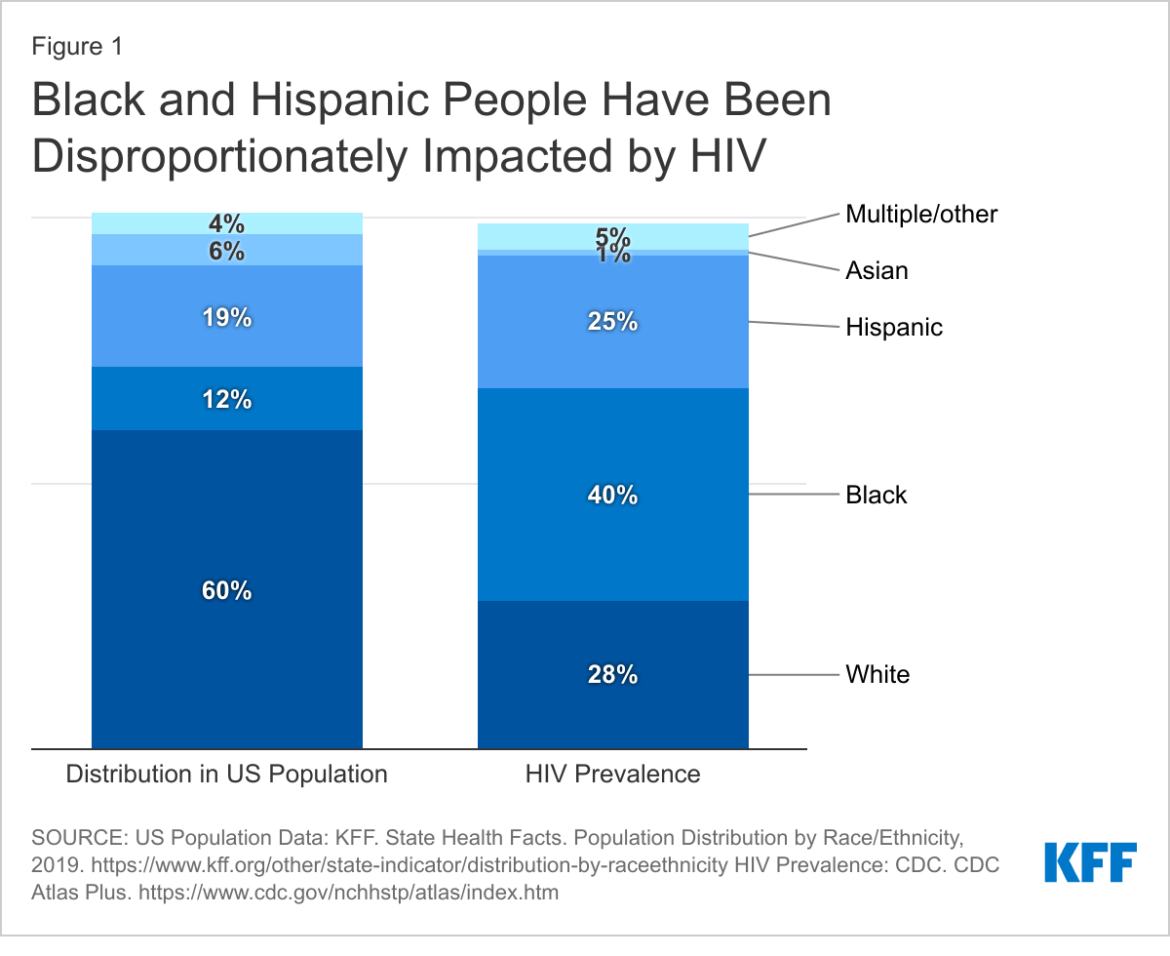
“Black people represented 13% of the U.S. population, but 40% of people with HIV. Hispanics/Latinos represented 18.5% of the population, but 25% of people with HIV.”
— HIV.gov
“Effective prevention and treatment are not adequately reaching people who could benefit most,” according to HIV.gov.
Abbas, who has studied this illness throughout her 32-year career, saw this as a medical provider.
But strides have been made. The first treatments were sometimes worse than the disease, she said. Today scientists have honed in on what does and doesn’t work and continue to find ways to make treatment manageable on a day-to-day basis.
“That in itself is a revolution,” she said.
There are also more robust funding mechanisms. As a provider, she said the CDC’s latest guidelines removed restrictive barriers. Before, the onus was that physicians needed to take patients’ medical information to classify who could or could not be prescribed PrEP.
Now anyone who walks in the door can get a prescription.
Then there are nonprofit centers like BlaqOut in Kansas City. BlaqOut works to break stigmas among Black Men who have Sex with Men (BMSM), to help them access care more readily.
The organization provides free testing, support and a safe space for Black queer men.
Editor’s note: The “Flatland in Focus” program’s host D. Rashaan Gilmore also is CEO of BlaqOut. In this month’s episode airing on Kansas City PBS, Gilmore leads the panel discussion on HIV/AIDS with Sandy Woodson, director of the “AIDS in KC: The Early Days” documentary, two guests living with HIV and Dr. Ume Abbas, a physician with a breadth of HIV-specific research experience.
‘Will I be able to still function properly?’
BlaqOut is where Quintez Fox first found the support network – and treatment – he needed.
A soft-spoken 33-year-old, Fox never expected to get an HIV-positive result.
Especially not at 19.
Today, he’s being treated. But even with the advent of new medications, the difficulties he faces have to do with long-lasting stigmas and transparency among peers.
It’s taken a psychological toll. He gets anxiety and depression.

People hesitate to talk about HIV, he said. In his circles, it’s on a need-to-know basis if at all. Though he considers his friend group to be open and supportive, he knows others his age aren’t or are dismissive of the risks.
He also has an added perspective. Fox worked in a nursing home where he met elderly folks who were HIV-positive. This got him thinking about his future health.
“Even though people say you can live with this, as you get older, a lot of things start to change in your body,” Fox said. “I kind of have those fears. When I’m 50 will I be able to still function properly?”
This concern reverberates across generations, especially among those living with HIV in their 50s today. Keyes knows her health could dip at any point, for instance.
A national leader in AIDS advocacy and education put it like this in a New York Magazine interview in 2009: “Aging is the No. 1 problem in HIV today.”
At the height of the AIDS crisis, the average lifespan for folks diagnosed with HIV or AIDS was six to 12 months. Today, the lifespan is 10 years from the time they are diagnosed.
“If a young person with newly acquired HIV begins antiretrovirals, almost immediately we can expect to have a normal lifespan,” Abbas said.
Fox is young and mostly healthy now. But he feels the effects of his diagnosis and the medications he takes on a daily basis.
“I get sleepy after taking the pills,” he said. “It’s like clockwork.”
27% of Black and 31% of Hispanic/Latino men were using pre-exposure prophylaxis (PrEP), compared with 42% of White men.
– CDC
While grateful for his treatment, medication is a double-edged sword. Some can access it, others cannot. And sometimes, it can be expensive.
Then there are those who take preventative medication. Fox sees a lack of discretion among those who take pre-exposure prophylaxis – also known as PrEP.
He is concerned medications like PrEP give folks a false sense of security. He feels it has to do with a lack of honest communication.
“That’s also how I ended up in this situation,” Fox said. “A friend of mine knew that the guy was positive. And his reasoning for not saying anything to me is because it was his business.”
Being open about status is key, and continues to be. As a result, testing would be less taboo. Taking time off from work to get checked would be more encouraged.
And maybe then, it would encourage friend groups to serve as a safety net.
“I wish there was a way to make people feel comfortable,” he said.
Fear, Education and Community
Before HIV or AIDS had a name, it was known as “gay cancer,” recalled Eduardo, whose name has been changed for this story to protect his medical privacy. Like Keyes, he tested positive in the early 1990s.
“I consider myself a dinosaur,” Eduardo said.
When he was 26, he moved to Los Angeles.
An openly gay, Latino creative, he moved from Kansas to California for a chance to break into the entertainment industry. He got his big break and worked with celebrities such as Arnold Schwarzenegger and Cher.
It was the 1990s and as word spread about this new disease taking his community by storm, he tested often.
All it took was letting his guard down one night and partying “a bit too much.” Cases were on the rise and then the reality of the crisis crystallized for him.
The same day Eduardo got his results, his friend Michael was admitted to a hospital with AIDS-related complications. Several months later, Michael died.
He knew many like Michael who didn’t want to get tested for fear of social stigmas. Unlike Eduardo, who wanted to know his status, Michael put off tests until one day his illness had progressed to AIDS.
AIDS in KC: The Early Days | A Kansas City PBS Documentary
Michael lived in Kansas where family members kept him away from his life partner and disapproved of his sexual orientation.
Acceptance or a lack of can make or break a person.
So, Eduardo found a community to rely on, to talk to and learn from. He said that was his lifeline, even if just two of them are alive today.
“I made a promise to myself. I don’t know what it would be that would take me out of this life, but it wasn’t going to be HIV and AIDS,” Eduardo said.
At the same time, he asked himself: “If you died tomorrow, are you going to die happy? Every time since that point, as a 26-year-old kid, I am still answering ‘yes’ every day.”
Since his diagnosis, he’s been a leader in HIV/AIDS advocacy and education.
To this day, Eduardo’s mission is to open the lines of communication among younger folks. He gets how difficult it can be to share one’s status but health should be supported by the community rather than in solitude.
He is certain that intergenerational connections can safeguard against risky behaviors. When he recalls his days in California, he leaned on acquaintances he calls his “gay parents” in L.A. The lessons they shared he passes on.
In turn, people like his 21-year-old niece and her friends can learn from him. But opening up requires trust.
His message to younger folks: “Just educate yourself about your health. And talk.”
Vicky Diaz-Camacho covers community affairs for Kansas City PBS. Sandy Woodson is the producer of “AIDS in KC: The Early Days,” now airing on KCPBS.




